Translate this page into:
A Leap above Friedewald Formula for Calculation of Low-Density Lipoprotein-Cholesterol
Address for correspondence: Dr. Reema Kapoor, E-mail: kapoor.reema25@gmail.com
This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Purpose:
The purpose was to compare the different calculated methods of low-density lipoprotein cholesterol (LDL-C) estimation and to determine which of them correlate best with the direct method.
Materials and Methods:
The records of 480 samples for lipid profile were analyzed. Apart from the direct method, LDL-C was calculated by Friedewald low-density lipoprotein cholesterol method (F-LDL-C), modified Friedewald low-density lipoprotein cholesterol method (MF-LDL-C), and Anandaraja low-density lipoprotein cholesterol method (A-LDL-C). Paired t-test and Pearson correlation were evaluated between the different methods. Degree of agreement between the calculated methods and direct method was detected by Bland–Altman graphical plots.
Results:
A strong correlation was found between all calculated LDL-C methods and direct low-density lipoprotein cholesterol method (D-LDL-C) assay, that is, F-LDL-C versus D-LDL-C = 0.94; A-LDL-C versus D-LDL-C = 0.93 and MF-LDL-C versus D-LDL-C = 0.95. No statistically significant difference was found between D-LDL-C and MF-LDL-C. Bland–Altman plot for MF-LDL-C showed minimal negative bias.
Conclusions:
The study pointed out that MF-LDL-C correlated maximally with D-LDL-C estimation at all levels of triglycerides and MF-LDL-C can be used in place of D-LDL-C when the direct method cannot be afforded.
Keywords
Anandaraja
Friedewald
low-density lipoprotein cholesterol
modified Friedewald
INTRODUCTION
Coronary heart disease (CHD) accounts for the greatest number of deaths and disability worldwide, and burden of CHDs is on the rise in low-middle income countries (LMICs).[1] However, these deaths can be prevented if the risk is diagnosed accurately. The relationship between serum low-density lipoprotein cholesterol (LDL-C), which correlates highly with total cholesterol (TC), and CHD risk has been observed throughout the world. It has been identified as a major risk factor for CHD, and hence the primary target of cholesterol-lowering therapy as per reports of The adult treatment panel.[2] It has been found that for every 1% reduction in LDL-C, the relative risk for major CHD events is reduced by nearly 1%.[2] Hence, the accurate and standardize measurements of LDL-C are required for reliable classification of patients.
Recommendations for measurement of LDL-C were issued by a National Cholesterol Education Program (NCEP) expert laboratory panel in 1995.[3] The panel recommended standardization of the measurements, that is, achieving traceability of all results to accepted reference methods (RMs). The Centre for Disease Control and Prevention (CDC) uses β-quantification as an RM, based on the Lipid Research Clinics (LRC). But the β-quantification procedure is costly, labor intensive, time-consuming, not available everywhere and can be performed only on few samples a day. Hence, its use is not feasible in routine laboratory especially in LMICs.[4] Direct homogeneous assays have been developed for the measurement of LDL-C levels. These have shown reasonable accuracy and precision as compared to RM. NCEP and Cholesterol Reference Method Laboratory Network of CDC certified commercially available direct LDL-C kits, and these have been available for use in routine clinical laboratories.[5] But being costly, they are still not used in most of the Indian laboratories.[4]
Since LDL is important in CHD risk assessment, the measurement of LDL should be accurate, and it should be cost-effective for the general population.[6] Most laboratories in LMICs estimate LDL-C levels with the Friedewald formula, based on the concentrations of TC, high-density lipoprotein cholesterol (HDL-C), and triglycerides (TGs).[7] Friedewald et al. described a formula to estimate LDL-C as an alternative to tedious ultracentrifugation. The calculation was actually proposed for use in epidemiologic studies but was later rapidly adopted and became the method of choice by routine clinical laboratories, in part for economic reasons.[3] Shortcomings of the procedure were addressed in the original publication.[7] These includes: Overestimation of very low-density lipoprotein cholesterol (VLDL-C) and underestimation of LDL-C due to presence of chylomicrons, calculation requires a fasting specimen (ideally 12 h fasting), calculation was recommended only for specimens with TGs up to 400 mg/dL, not useful in type III hyperlipidemia or dysbetalipoproteinemia. A major disadvantage in calculating LDL by Friedewald method is that the variability is a product of the combined variabilities in the three underlying measurements. In routine laboratories, variability appeared to be much higher (12%) as compared to variability in experienced and well-standardized lipid laboratories (4%), as observed by The NCEP Expert Panel.[4] Other limitations are underestimation of LDL-C in patients with diabetes mellitus, end-stage renal disease, hepatic failure and patients on hormone replacement therapy.[4] Moreover, LDL cholesterol includes intermediate density lipoprotein (IDL) and lipoprotein (a) in it. Increased concentration of IDL and Lp (a) are also associated with increased risk of CHD. But because of their small concentration (a few mg/dL), NCEP working group on LDL cholesterol measurement suggested that LDL cholesterol value should not be corrected for the contribution of other atherogenic lipoproteins.[8]
Attempts have been made to evaluate and refine Friedewald's original formula. Anandaraja et al. proposed another method for calculating LDL-C.[9] It does not require HDL-C result for the calculation and hence can prove to be more cost-effective. Since it uses only two analytes chances of analytical errors are decreased.[9] This formula has been approved in Brazilian and Greek population.[10] However, studies found that there was no advantage of Anandaraja's formula over Friedewald formula for estimation of LDL-C by calculation.[11]
Another modification in original Friedewald's formula for calculation of LDL was given by Puavilai and Laoragpongse[12] which assumes that VLDL constitutes one-sixth of total TGs and it is costly for serum LDL test from direct measurement, especially if it has to be tested several times in a year. The authors found modified formula to be more accurate than the original formula in estimation of LDL-C. It also partially overcame the problems of fasting, presence of diabetes, obesity and familial hypertriglyceridemia unlike seen with original Friedewald formula. The study was done in Thai population. The literature on the use of this modified Friedewald formula among Indian population is not available. Against this background, the present study was conducted (i) To determine that which of these calculated formulae (original Friedewald, Anandaraja and modified Friedewald) show maximum correlation with direct low-density lipoprotein cholesterol method (D-LDL-C) estimation at different serum TG levels in Indian population. (ii) To find the actual agreement between these methods.
MATERIALS AND METHODS
Data collection
We reviewed records of blood samples which were sent to our Clinical Biochemistry Laboratory, Department of Biochemistry, Lok Nayak Jai Prakash hospital, New Delhi for the estimation of fasting lipid profile. Secondary data of 480 patients were collected after obtaining prior permission from the concerned authority. The reviewed records referred to the period during May 2013 to October 2013. As a routine procedure, the samples were collected after 10–12 h of overnight fast by withdrawing 3 ml of venous blood in plain vial. The samples were centrifuged at 3000 rpm for 15 min to obtain serum and were analyzed for lipid profile on the same day.
Serum cholesterol was estimated by cholesterol oxidase-peroxidase method using a commercial kit from Beckman Coulter on Beckman Coulter DXC (Beckman Coulter Ireland, Inc., Mervue Business Park, Mervue, Galway, Ireland 353 91 774068. Beckman Coulter, Inc. 250 S. Kraemer Blvd., Brea, CA 92821 U.S.A.) analyzer with a coefficient of variation (CV) of 3%.[13] Serum TG was estimated by glycerol-3 phosphate oxidase-3,5-dichloro-2-hydroxybenzenesulfonic acid method on the same analyzer using a commercial kit from Beckman Coulter with a CV of 3%.[14] HDL-C was estimated by a commercial kit from Beckman Coulter based on homogenous method (with a CV of 3%) using a detergent which solubilizes only the HDL lipoprotein particles and releases HDL cholesterol to react with cholesterol esterase and cholesterol oxidase in the presence of chromogens to produce a color product.[15]
Direct low-density lipoprotein cholesterol estimation
Low-density lipoprotein cholesterol was estimated by direct homogenous method of Daiichi Pure Chemicals, Tokyo by using a commercial kit from Beckman Coulter on DXC analyzer with a CV of 2%. Homogenous method of LDL-C depends on unique detergent which solubilizes only the non-LDL lipoproteins and releases cholesterol to react with cholesterol esterases and oxidases to produce a noncolor forming reaction. A second detergent solubilizes the remaining LDL particles, and a chromogenic complex allows for color formation.[16]
Low-density lipoprotein reagent is used to measure cholesterol concentration by a timed endpoint method. The change in absorbance is read at 560 nm. The change in absorbance is directly proportional to the concentration of cholesterol in the sample.
Calculated low-density lipoprotein cholesterol estimation
Apart from above method, LDL cholesterol was calculated by following formulae:
-
Friedewald: Friedewald low-density lipoprotein cholesterol (F-LDL-C) = TC − (TG/5 + HDL-C)
-
Modified Friedewald: Modified Friedewald low-density lipoprotein cholesterol (MF-LDL-C) = TC − (TG/6 + HDL-C)
-
Anandaraja: Anandaraja low-density lipoprotein cholesterol (A-LDL-C) = (0.9 × TC) − (0.9 × TG/5) − 28.
Statistical analysis
Data were entered into Microsoft Office Excel 2007. Discrete data were reported as mean and standard deviation. Paired t-test and Pearson correlation were performed to find the significant difference and correlation in LDL-C concentration obtained by a direct method and different calculations, respectively. The level of significance was taken as P < 0.05. To examine the degree of agreement between the values obtained by the two methods, Bland–Altman graphical plots were used. The mean percentage difference (PD) was calculated using the formula: PD calculated LDL-C = (calculated LDL-C − D-LDL-C)/D-LDL-C × 100. Data collected were classified into three groups according to the serum TG concentrations (mg/dL) as group A: TG - 200 mg/dL and below, group B: TG - 201–400 mg/dL, and group C: TG - 400 mg/dL and above. The performance of the three formulae was compared at different levels of TG.
RESULTS
The comparative study was done on lipid profile records of 480 patients. There were 320, 138, and 22 patients in group A, B, and C, respectively. The mean LDL-C levels (mg/dL) were 117.02, 106.63, 102.25, and 113.00 for D-LDL-C, F-LDL-C, A-LDL-C, and MF-LDL, respectively [Table 1]. No statistically significant difference was found in the mean of LDL-C calculated by modified Friedewald method as compared to direct LDL-C.
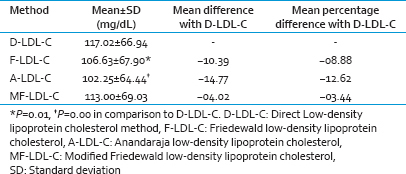
The calculated formulae underestimate LDL-C by 10.39 mg/dL, 14.77 mg/dL and 04.02 mg/dL by Friedewald's, Anandaraja's and modified Friedewald's method, respectively, in comparison to the direct method. On calculating the mean PD, it was found that MF-LDL-C differs by 3.44% from the D-LDL-C which was much lower in comparison to the other two calculated formulae (8.88% and 12.62% by F-LDL-C and A-LDL-C, respectively) [Table 1].
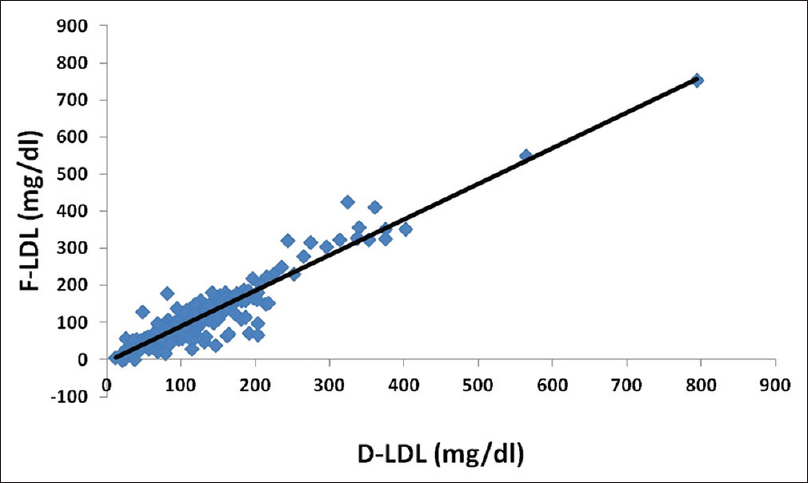
A strong correlation was found between all calculated LDL-C methods and D-LDL-C assay, that is, F-LDL-C versus D-LDL-C = 0.94 [Figure 1]; A-LDL-C versus D-LDL-C = 0.93 [Figure 2] and MF-LDL-C versus D-LDL-C = 0.95 [Figure 3].
- Scatter plot of Anandaraja low-density lipoprotein cholesterol against direct low-density lipoprotein cholesterol. There was a correlation of r = 0.93
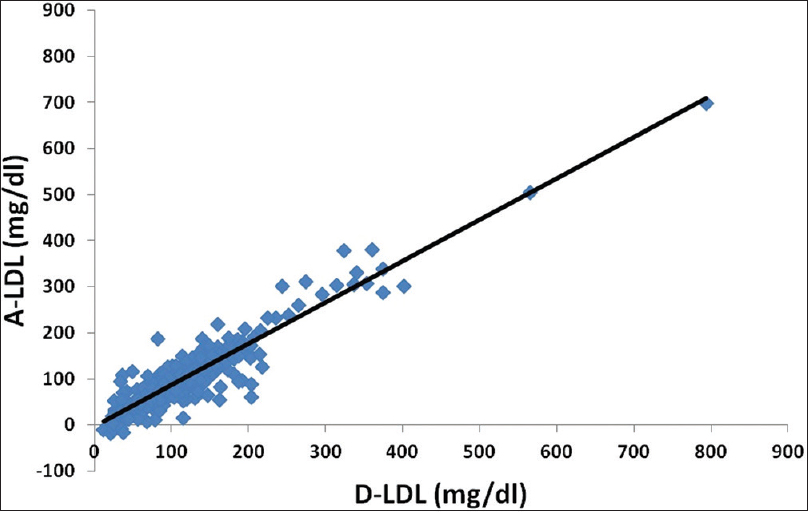
- Scatter plot of Anandaraja low-density lipoprotein cholesterol against direct low-density lipoprotein cholesterol. There was a correlation of r = 0.93
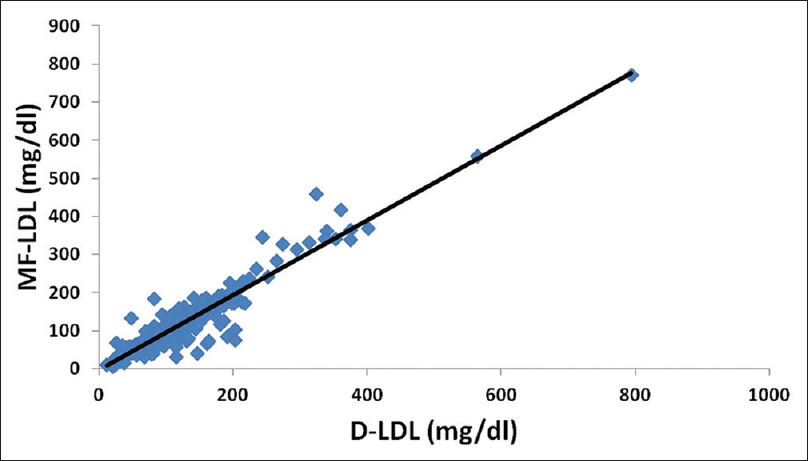
- Scatter plot of modified Friedewald low-density lipoprotein cholesterol against direct low-density lipoprotein cholesterol. There was a correlation of r = 0.95
To find the agreement between the direct and calculated LDL methods, Bland–Altman Plot was prepared [Figures 4–6] but the negative bias in them indicates that although they correlate to one another they cannot be used in place of direct LDL except the modified Friedewald method where the negative bias was minimum.
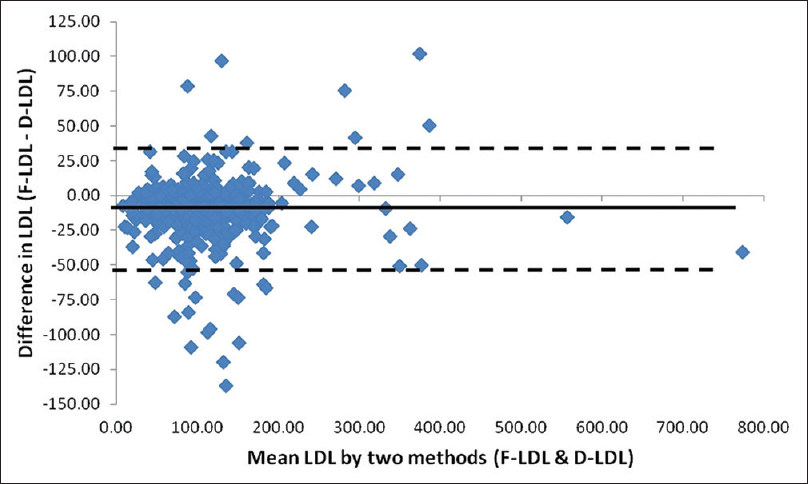
- Bland–Altman plot for low-density lipoprotein cholesterol estimated directly and by Friedewald's calculation. Mean: −10.39 (negative bias), standard deviation (SD): 22.18; mean +2 SD: +33.97; mean −2 SD: −54.75
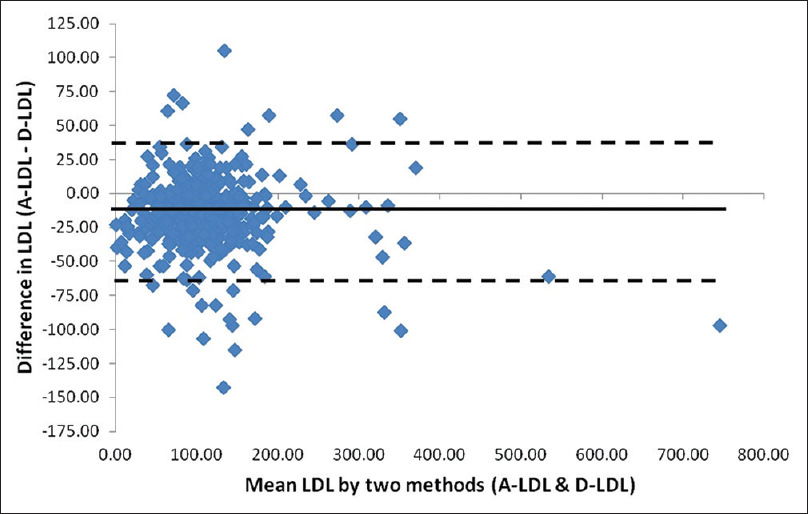
- Bland–Altman plot for low-density lipoprotein cholesterol estimated directly and by Anandaraja's calculation. Mean: −14.77 (negative bias), standard deviation (SD): 24.82; mean +2 SD: +34.87; mean −2 SD: −64.41
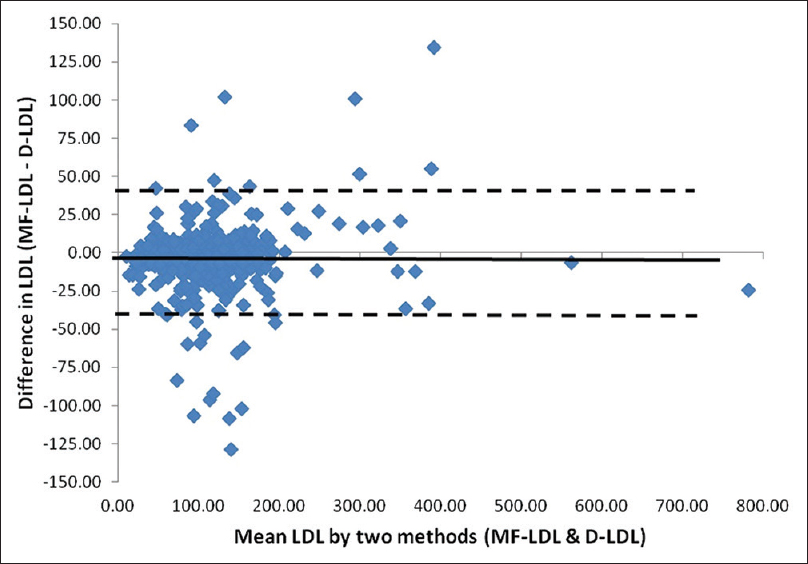
- Bland–Altman plot for low-density lipoprotein cholesterol estimated directly and by modified Friedewald's calculation. Mean: −4.02 (negative bias), standard deviation (SD): 21.46; mean +2 SD: +38.90; mean −2 SD: −46.94
Comparison of LDL-C at different levels of TGs did not show statistically significant difference between D-LDL-C and calculated LDL-C by Friedewald and Modified Friedewald's method (F-LDL-C and MF-LDL-C) [Table 2]. At TG < 200 mg/dL and TG: 201-400 mg/dL, a significant difference was found between measured LDL-C and calculated LDL-C by Anandaraja's method (A-LDL-C).

DISCUSSION
Coronary heart disease is one of the most prevailing causes of morbidity and mortality.[17]
In LMICs, Friedewald formula is commonly used to estimate LDL-C in routine laboratories, despite its several limitations. There were no limitations proposed with Anandaraja's formula but as said earlier, no advantage was found over Friedewald's formula by authors.[11] To the best of author's knowledge, this is the first study in which modified Friedewald formula given by Puavilai et al. was evaluated in India, and comparison was made with original Friedewald formula and Anandaraja's formula.
Our study pointed that there was a good correlation between all calculated LDL methods and direct method. There was a correlation of 0.94 between D-LDL-C and Friedewald LDL in our study which was in concordance of other studies which say it to be ranging from 0.78 to 0.93.[51118] The correlation between D-LDL-C and A-LDL-C in our study was found to be 0.93 which was similar to other studies, that is, correlation of 0.93, 0.89, and 0.81.[51119] Our study found a correlation of 0.95 between MF-LDL-C and D-LDL-C, which was higher than the one found by Kamal et al (r = 0.81).[5]
Even if there was a positive correlation but to find the actual relation between these methods Bland–Altman plot was calculated, which revealed negative bias. This suggests that there is the difference in results obtained by calculated and direct method. Similar finding of negative bias was reported in the study by Gupta et al.[11] The reason of negative bias was that there was underestimation of calculated LDL from direct LDL. This underestimation was 10.39%, 14.77%, and 04.02% by Friedewald, Anandraja and modified Friedewald respectively in our study. Similar findings were reported by Gupta et al.[11] that there is underestimation of 10% and 14% with Friedewald and Anandaraja methods, respectively. However, Kamal et al.[5] found underestimation of 17% and 22% by Friedewald and Anandaraja methods, respectively. On the other hand, Kamezaki et al.[20] reported underestimation of only 5.9% with Friedewald formula. The calculation of mean PD of three calculated methods from the direct method suggested that the difference was least with the modified Friedewald method as compared to others, that is, 08.88%, 12.62%, and 03.44% for Friedewald, Anandaraja, and modified Friedewald, respectively. Similar differences were reported in the study by Gupta et al.[11] where it was 8.8 and 11.4% for Friedewald and Anandaraja, respectively. However, in the study by Vujovic et al.,[19] these differences were found to be 6.9 and 3.9% for Friedewald and Anandraja methods, respectively. Kamal et al.[5] also studied difference of modified Friedewald method in addition, and reported differences were 16.7%, 22.35%, and 10.5% for Friedewald, Anandaraja, and modified Friedewald, respectively, that is, least with modified Friedewald method.
Since the negative bias was maximum for Anandaraja formula, so if this is used many cases of CHD may be denied of early initiation of treatment. Direct methods are accurate and precise for estimation of LDL but when LDL is to be frequently measured in monitoring of CHD, it adds to the cost of treatment.
CONCLUSION
Keeping in mind that LDL calculated by modified Friedewald formula correlates well with direct LDL so to monitor treatment of patients of CHD (i.e. decrease in LDL-C and TG and increase in HDL) it should be used in place of Friedewald formula in routine laboratories for calculation of LDL.
Source of Support: Nil.
Conflict of Interest: None declared.
REFERENCES
- World Health Organization. Global Atlas on CVD Prevention and Control. Geneva: WHO; 2011.
- [Google Scholar]
- Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel III guidelines. Circulation. 2004;110:227-39.
- [Google Scholar]
- National Cholesterol Education Program recommendations for measurement of low-density lipoprotein cholesterol: Executive summary. The National Cholesterol Education Program Working Group on Lipoprotein Measurement. Clin Chem. 1995;41:1414-20.
- [Google Scholar]
- Methods for measurement of LDL-cholesterol: A critical assessment of direct measurement by homogeneous assays versus calculation. Clin Chem. 2002;48:236-54.
- [Google Scholar]
- A comparison of calculated with direct measurement of low density lipoprotein cholesterol level. Journal of Chittagong Medical College Teacher's Association. 2009;20:19-23.
- [Google Scholar]
- Is Friedewald formula a good estimation for low density lipoprotein level in Iranian population? J Res Med Sci. 2012;17:519-22.
- [Google Scholar]
- Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clin Chem. 1972;18:499-502.
- [Google Scholar]
- Measurement of lipids, lipoproteins and apolipoproteins. In: Burtis CA, Ashwood ER, Bruns DE, eds. Teitz Textbook of Clinical Chemistry and Molecular Diagnosis (4th ed). St. Louis, Missouri: Elseviers Saunders; 2006. p. :938-52.
- [Google Scholar]
- Low-density lipoprotein cholesterol estimation by a new formula in Indian population. Int J Cardiol. 2005;102:117-20.
- [Google Scholar]
- Low-density lipoprotein cholesterol estimation by the Anandaraja's formula – Confirmation. Lipids Health Dis. 2006;5:18.
- [Google Scholar]
- Does LDL-C estimation using Anandaraja's formula give a better agreement with direct LDL-C estimation than the Friedewald's formula? Indian J Clin Biochem. 2012;27:127-33.
- [Google Scholar]
- Is calculated LDL-C by using the new modified Friedewald equation better than the standard Friedewald equation? J Med Assoc Thai. 2004;87:589-93.
- [Google Scholar]
- Quantitative determination of serum triglycerides by the use of enzymes. Clin Chem. 1973;19:476-82.
- [Google Scholar]
- Dextran sulfate-Mg2+precipitation procedure for quantitation of high-density-lipoprotein cholesterol. Clin Chem. 1982;28:1379-88.
- [Google Scholar]
- Three generations of high-density lipoprotein cholesterol assays compared with ultracentrifugation/dextran sulfate-Mg2+method. Clin Chem. 1997;43:816-23.
- [Google Scholar]
- Journey in guidelines for lipid management: From adult treatment panel (ATP)-I to ATP-III and what to expect in ATP-IV. Indian J Endocrinol Metab. 2013;17:628-35.
- [Google Scholar]
- Comparison of two methods of estimation of low density lipoprotein cholesterol, the direct versus Friedewald estimation. Indian J Clin Biochem. 2005;20:54-61.
- [Google Scholar]
- Evaluation of different formulas for LDL-C calculation. Lipids Health Dis. 2010;9:27.
- [Google Scholar]
- A direct measurement for LDL-cholesterol increases hypercholesterolemia prevalence: Comparison with Friedewald calculation. J UOEH. 2010;32:211-20.
- [Google Scholar]





